Scientists recently developed a breakthrough therapy that clears toxic proteins from nerve cells—a discovery that could transform the treatment of motor neuron disease (MND).
About Motor Neuron Disease
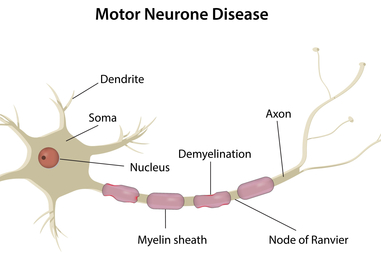
Motor neuron disease (MND) is a group of rare, progressive neurological disorders that damage motor neurons, the nerve cells that control voluntary muscles. This damage leads to muscle weakness, a gradual loss of movement, and eventually paralysis.
Key Aspects of Motor Neuron Disease
- Progressive Nature: MND is progressive, meaning symptoms worsen over time as more motor neurons die. It can significantly shorten life expectancy, particularly in forms like Amyotrophic Lateral Sclerosis (ALS), but the rate of progression varies widely among individuals.
- Unaffected Senses: In most cases, MND does not affect a person's senses (sight, hearing, touch, taste, smell), bladder or bowel function, or sexual function.
- Multidisciplinary Care: While there is no cure, a multidisciplinary healthcare team can help manage symptoms, maintain independence, and improve quality of life.
Types of Motor Neuron Disease
MNDs are classified by which motor neurons (upper in the brain, lower in the brainstem and spinal cord, or both) are affected and how they progress.
| Type |
Affected Neurons |
Key Symptoms |
Prognosis |
| Amyotrophic Lateral Sclerosis (ALS) |
Both upper and lower |
Muscle weakness, stiffness, twitching, slurred speech, difficulty breathing/swallowing |
Most common; life expectancy typically 2-5 years after onset |
| Progressive Bulbar Palsy (PBP) |
Brainstem (bulbar) region |
Difficulty speaking/swallowing, choking spells, emotional lability (inappropriate crying/laughing) |
Shorter survival time than ALS on average |
| Progressive Muscular Atrophy (PMA) |
Lower motor neurons |
Slow, progressive muscle wasting and weakness, particularly in arms/legs, no upper motor neuron signs |
Slower progression than ALS; generally not fatal in early stages but can progress to ALS |
| Primary Lateral Sclerosis (PLS) |
Upper motor neurons |
Muscle stiffness (spasticity) and weakness, typically in the legs first, progressing slowly |
Very slow progression; usually not life-shortening |
| Spinal Muscular Atrophy (SMA) |
Lower motor neurons |
Inherited, affects children and adults with muscle weakness, often in trunk/limbs |
Severity varies by type; some forms are life-threatening in infancy |
| Kennedy's Disease |
Lower motor neurons |
Inherited (affects men), muscle cramps/twitches, weakness in face/limbs, endocrine issues |
Very slow progression, not life-shortening |
Symptoms
Early symptoms are often subtle and vary, but generally involve progressive, painless muscle weakness.
Common symptoms include:
- Weakened grip or stumbling/clumsiness.
- Muscle twitching (fasciculations) and cramps.
- Slurred speech or difficulty swallowing.
- Breathing difficulties and fatigue.
- Emotional lability (uncontrollable crying or laughing).
Causes
- The exact causes of most MND cases are unknown (sporadic cases account for 90-95%). A combination of genetic, environmental, and lifestyle factors is thought to play a role.
- Genetics: About 5-10% of cases are inherited due to specific gene mutations.
- Risk Factors: Age (typically diagnosed between 40 and 70), male sex, smoking, and exposure to certain toxins or heavy metals may increase risk.
Diagnosis
Diagnosis is challenging in the early stages as symptoms overlap with other conditions. A neurologist will use a combination of methods to rule out other diseases:
- Thorough medical history and physical examination.
- Electromyography (EMG) and nerve conduction studies (NCS): Measure electrical activity in muscles and nerves.
- MRI scans: Used to rule out structural issues, tumors, or other neurological conditions like multiple sclerosis.
- Blood and urine tests: To exclude metabolic or inflammatory causes.
Treatment and Management
There is no cure for MND, but treatments focus on managing symptoms and supporting quality of life.
- Medications: Drugs like riluzole (Rilutek) and edaravone (Radicava) may slightly slow the progression of ALS. Other medications can help with muscle stiffness, cramps, pain, and excessive saliva.
- Therapies: Physical, occupational, and speech therapy are vital for maintaining mobility, function, and communication.
- Supportive Care: Assistive devices (braces, wheelchairs, communication aids), nutritional support (feeding tubes if necessary), and respiratory support (non-invasive ventilation) are essential components of care.
Download Pdf